Health
Senate continues probe on PhilHealth’s ‘misappropriated funds’
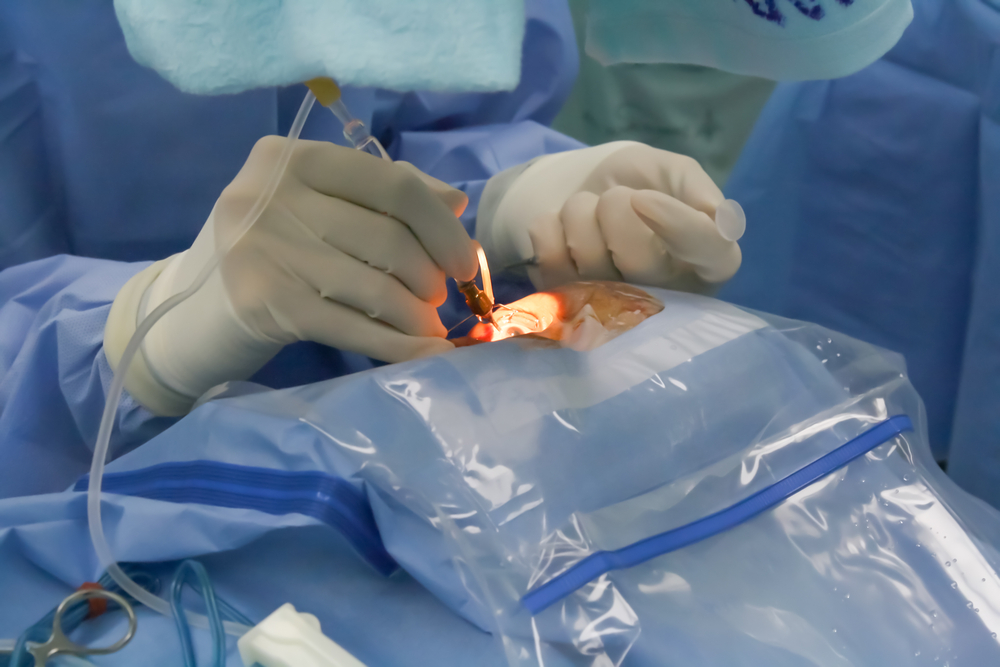
Of the alleged P2 billion misappropriated PhilHealth funds, P325 million of this was given to two eye centers alone (Shutterstock image)
MANILA – The Senate Blue Ribbon committee will continue its investigation on Wednesday regarding the P2 billion alleged misappropriated funds of the Philippine Health Insurance Corp. (PhilHealth) by various accredited hospitals and clinics.
Invited to attend tomorrow’s probe are Department of Health (DOH) Secretary Janette Garin, PhilHealth President Alexander Padilla, Philippine Medical Association President Minerva Calimag and Philippine Eye Bank President Minguita Padilla, among others.
The Senate investigation was initiated when PhilHealth grew suspicious of the large claims of sums requested by several accredited healthcare facilities throughout the country.
Blue Ribbon committee chairman Teofisto Guingona III disclosed that he was disturbed and angered with the ongoing ‘hakot’ mechanism wherein some PhilHealth members would undergo unnecessary operations just so hospitals and clinics could claim money from the country’s premier health insurance provider.
Guingona stressed the dangers patients were exposed to through these unneeded treatments.
“If found true, this is a matter of national concern. It is criminal to misappropriate funds that are actually needed by other patients. But to endanger the lives of Filipinos as a means to eat through PhilHealth’s funds is beyond deplorable,” Guingona said.
“We are therefore conducting an inquiry on this matter to ensure that PhilHealth, as the country’s premier health insurance provider, would have adequate policing mechanisms that will promote transparency and accountability among health care providers,” he added.
Benefit payments to healthcare facilities have already amounted to P2 billion, with P325 million of this given to two eye care centers alone mostly for cataract procedures.
“We must get to the bottom of these right away to ensure that the funds of PhilHealth are protected from unscrupulous parties,” Guingona said.
“If the allegations are true, then greed would have taken over a good program. At the end of the day, PhilHealth funds are the people’s money. This is because part of its funds comes from members’ contributions and from government,” he added.
While there are bulk cases of unnecessary operations, there are also reports of unperformed operations to other PhilHealth members.





















Pingback: Senate hears cataract patients’ plight » Philippine Canadian Inquirer